Search This Blog
Your go-to resource for gut health, hormone balance, and natural wellness solutions. Learn science-backed strategies for digestive health, post-antibiotic recovery, and optimal performance.
Featured
- Get link
- X
- Other Apps
The Gut-Hormone Connection: How Your Gut Controls Your Estrogen Levels
last updated: 20/03/2025
Author: Catherine
The gut microbiome, a complex ecosystem of trillions of microorganisms residing in the digestive tract, has been increasingly recognized for its influence on various aspects of human health. Among its many functions, the gut microbiome plays a crucial role in hormone regulation, particularly estrogen metabolism. This relationship between gut bacteria and estrogen has led to the identification of specific microbial communities, known as the estrobolome or estrobiome, that directly impact hormone levels and, consequently, women's health.
What is the Estrobolome?
The estrobolome, also referred to as the estrobiome in some research, is the collective term for the subset of gut bacteria that are capable of metabolizing estrogens. These bacteria possess specific enzymatic activities that influence whether estrogens are reabsorbed into circulation or excreted from the body. The estrobolome represents a critical component of the body's hormone regulation system, particularly in women, where estrogen plays fundamental roles in reproductive health, bone density, cardiovascular function, and cognitive processes.
The concept of the estrobolome highlights the bidirectional relationship between sex hormones and gut microbiota: estrogens shape the composition of gut bacteria, while these bacteria, in turn, regulate estrogen levels. This intricate relationship forms the basis of the gut-hormone axis, a communication network that significantly impacts women's health across various life stages.
How Gut Bacteria Regulate Estrogen
Estrogen metabolism involves a complex series of processes that occur primarily in the liver, where estrogens are conjugated (bound to other molecules) to facilitate their excretion through bile into the intestines. This process renders estrogens inactive and prepares them for elimination from the body. However, the estrobolome can fundamentally alter this pathway.
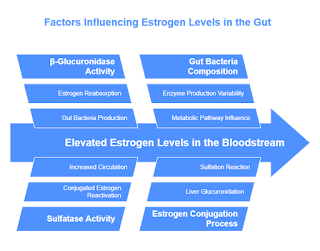
The Role of β-Glucuronidase and Sulfatase Enzymes
The primary mechanism through which gut bacteria influence estrogen levels involves the production of specific enzymes:
-
β-Glucuronidase: This enzyme, produced by various gut bacteria, deconjugates estrogens by removing the glucuronic acid that was attached during liver metabolism. This deconjugation process reactivates estrogens, allowing them to be reabsorbed into circulation rather than excreted.
-
Sulfatase: Similar to β-glucuronidase, sulfatase enzymes remove sulfate groups from conjugated estrogens, also resulting in the reactivation and potential reabsorption of estrogens.
The activity levels of these bacterial enzymes significantly determine the amount of estrogen that remains in circulation versus the amount that is eliminated from the body. Higher enzyme activity leads to increased deconjugation, greater reabsorption of estrogens, and consequently, elevated estrogen levels in the bloodstream.
Key Bacterial Players in Estrogen Metabolism
Research has identified several bacterial species and families that contribute significantly to estrogen metabolism:
-
Bacteroides: These gram-negative bacteria are among the most abundant in the human gut and have been associated with β-glucuronidase activity.
-
Bifidobacterium: Generally considered beneficial bacteria, certain Bifidobacterium species influence estrogen metabolism.
-
Escherichia coli: These common gut bacteria produce β-glucuronidase and can influence estrogen reactivation.
-
Lactobacillus: Known for their probiotic properties, these bacteria may help maintain balanced estrogen metabolism.
-
Lachnospiraceae and Ruminococcaceae: These bacterial families, part of the Clostridia class, play significant roles in estrogen metabolism.
The balance and diversity of these and other bacterial populations determine the overall impact of the gut microbiome on estrogen levels. A diverse and balanced estrobolome generally supports healthy estrogen metabolism, while disruptions in these bacterial communities may lead to hormonal imbalances.
Signs and Symptoms of Estrobolome Imbalance
When the estrobolome becomes imbalanced—a condition known as dysbiosis—it can lead to inappropriate estrogen metabolism. This dysregulation may manifest as either estrogen excess (hyperestrogenism) or deficiency (hypoestrogenism), both of which can present with distinct symptoms and health implications.
Symptoms of Estrogen Excess
Estrogen dominance or excess may occur when there is elevated β-glucuronidase activity in the gut, leading to increased estrogen reabsorption. Symptoms may include:
- Heavy or painful menstrual periods
- Breast tenderness or fibrocystic breasts
- Bloating and water retention
- Mood swings, irritability, or anxiety
- Headaches, particularly premenstrually
- Weight gain, especially around the hips and thighs
- Decreased libido
- Fatigue
- Insomnia or sleep disturbances
Symptoms of Estrogen Deficiency
Conversely, insufficient estrogen levels, which can occur with certain gut imbalances or during menopause, may present with:
- Hot flashes and night sweats
- Vaginal dryness and discomfort
- Irregular or absent menstrual cycles
- Mood changes, including depression
- Poor concentration and memory issues
- Decreased bone density
- Joint pain
- Dry skin and reduced skin elasticity
- Urinary tract infections or incontinence
Health Conditions Associated with Estrobolome Dysbiosis
Disruptions in the gut-estrogen axis have been implicated in various health conditions affecting women:
Hormonal and Reproductive Disorders
-
Polycystic Ovary Syndrome (PCOS): Research suggests that women with PCOS often exhibit altered gut microbiota, which may contribute to hormonal imbalances characteristic of this condition.
-
Endometriosis: Estrogen plays a crucial role in the development and progression of endometriosis. Dysregulation of estrogen metabolism through gut dysbiosis may contribute to this condition.
-
Premenstrual Syndrome (PMS): Fluctuations in hormone levels, potentially exacerbated by estrobolome imbalances, may worsen premenstrual symptoms.
Metabolic and Inflammatory Conditions
-
Obesity: The gut microbiome influences metabolism and fat storage, and disruptions in the estrobolome may contribute to weight gain and obesity, particularly in women.
-
Type 2 Diabetes: Altered gut bacteria have been linked to insulin resistance and glucose metabolism, with estrogen playing a role in this relationship.
-
Cardiovascular Disease: Estrogen typically provides cardiovascular protection in premenopausal women. Dysregulation of estrogen metabolism may influence cardiovascular health.
Cancer Risk
-
Breast Cancer: Elevated estrogen levels represent a known risk factor for hormone-dependent breast cancer. The estrobolome's influence on circulating estrogen may affect this risk.
-
Endometrial Cancer: Similar to breast cancer, endometrial cancer risk is associated with estrogen exposure, which can be modulated by gut microbial activity.
Skin Health and the Gut-Skin Axis
The relationship between gut health and skin condition is increasingly recognized, with estrogen playing a mediating role:
- Estrogen affects skin thickness, hydration, and collagen production
- Gut dysbiosis may contribute to inflammatory skin conditions like acne and rosacea
- Changes in the gut microbiome during hormonal transitions (e.g., puberty, menopause) may influence skin health
Menopausal Transition
Research indicates that menopause significantly alters the gut microbiome:
- Reduced estrogen levels during menopause are associated with decreased gut microbial diversity
- These changes may contribute to menopausal symptoms and increased susceptibility to metabolic disorders
- The altered gut microbiome may affect bone health through reduced calcium absorption and increased inflammation
Factors Affecting the Estrobolome
Several lifestyle and environmental factors influence the composition and function of the estrobolome:
Dietary Influences
-
Fiber intake: Dietary fiber, particularly from fruits, vegetables, and whole grains, supports beneficial gut bacteria and promotes healthy estrogen elimination.
-
Fat consumption: High-fat diets, especially those rich in saturated fats, may negatively impact the estrobolome and promote estrogen reabsorption.
-
Protein sources: Plant proteins generally support a healthier gut microbiome compared to certain animal proteins.
-
Polyphenols: These plant compounds found in colorful fruits, vegetables, tea, and coffee support beneficial gut bacteria.
Medications and Supplements
-
Antibiotics: While sometimes necessary, antibiotics can disrupt the gut microbiome, including the estrobolome, potentially leading to hormonal imbalances.
-
Hormonal contraceptives: Birth control pills and other hormonal contraceptives can influence both estrogen levels and gut bacterial composition.
-
Probiotic and prebiotic supplements: These may help restore or maintain a healthy estrobolome.
Lifestyle Factors
-
Stress: Chronic stress affects gut function and bacterial composition, potentially disrupting estrogen metabolism.
-
Sleep quality: Poor sleep may alter the gut microbiome and hormone regulation.
-
Exercise: Regular physical activity generally supports a diverse and healthy gut microbiome.
Environmental Exposures
-
Xenoestrogens: Environmental chemicals with estrogen-like properties (found in certain plastics, pesticides, and personal care products) can disrupt the hormone system and potentially alter gut bacteria.
-
Pollution: Environmental pollutants may impact both gut health and hormone balance.
Optimizing the Estrobolome for Hormonal Balance
Several approaches may help maintain or restore a healthy estrobolome and support optimal estrogen metabolism:
Dietary Strategies
-
Increase fiber intake: Aim for 25-35 grams of fiber daily from diverse plant sources to support beneficial bacteria and promote estrogen excretion.
-
Consume fermented foods: Yogurt, kefir, sauerkraut, kimchi, and other fermented foods provide natural probiotics that may support the estrobolome.
-
Include phytoestrogens: Moderate consumption of foods containing plant estrogens (like flaxseeds, soy, and legumes) may help balance hormone levels.
-
Emphasize cruciferous vegetables: Broccoli, cauliflower, cabbage, and kale contain compounds that support healthy estrogen metabolism.
-
Limit alcohol consumption: Alcohol can disrupt both gut bacteria and estrogen metabolism.
Probiotic and Prebiotic Support
-
Probiotic supplements: Certain strains, particularly Lactobacillus and Bifidobacterium species, may support the estrobolome.
-
Prebiotic foods: Garlic, onions, leeks, asparagus, bananas, and oats contain prebiotic fibers that feed beneficial gut bacteria.
Lifestyle Modifications
-
Stress management: Practices such as meditation, yoga, and deep breathing can help maintain gut health and hormone balance.
-
Regular exercise: Moderate physical activity supports gut microbial diversity and healthy metabolism.
-
Adequate sleep: Prioritize quality sleep to support both gut health and hormone regulation.
-
Minimize exposure to environmental toxins: Choose natural personal care products and reduce plastic use when possible.
Future Directions in Estrobolome Research
The field of estrobolome research is rapidly evolving, with several promising areas of development:
-
Personalized approaches: Gut microbiome testing may eventually guide individualized recommendations for optimizing the estrobolome.
-
Targeted probiotics: Research is investigating specific bacterial strains that may help regulate estrogen metabolism.
-
Integration with conventional medicine: The estrobolome concept may increasingly inform approaches to treating hormonal conditions.
-
Expanded understanding of life-stage transitions: Further research will likely clarify how the estrobolome changes throughout a woman's life, from puberty through post-menopause.
Conclusion
The gut-hormone connection, specifically the role of the estrobolome in regulating estrogen levels, represents a significant aspect of women's health. Understanding this relationship provides new insights into the prevention and management of various hormonal imbalances and related conditions. By supporting gut health through diet, lifestyle, and targeted supplementation when necessary, women may optimize their estrogen metabolism and overall hormonal balance.
While research in this area continues to evolve, the current evidence strongly suggests that nurturing a healthy gut microbiome should be considered an essential component of women's health strategies across the lifespan. As always, women concerned about hormonal imbalances or related health conditions should consult with healthcare providers knowledgeable about both gut health and hormonal systems for personalized guidance.
Citations:
https://mattioli1885journals.com/index.php/actabiomedica/onlinefirst/view/15980
https://journals.plos.org/plosone/article?id=10.1371%2Fjournal.pone.0315576
https://www.ifm.org/articles/sex-hormones-and-the-gut-microbiome
https://www.frontiersin.org/journals/microbiology/articles/10.3389/fmicb.2024.1302819/full
- Get link
- X
- Other Apps
Popular Posts
The Gut-hormone Connection: New Insights into PCOS and Women's Health
- Get link
- X
- Other Apps

Comments
Post a Comment